Answers to Questions About Patient-Centered Primary Care Payment
- How would a primary care practice be paid under Patient-Centered Primary Care Payment?
- Wouldn’t it be simpler to pay primary care practices using a single per-member-per-month payment rather than three separate payments?
- Isn’t a risk-adjusted capitation or population-based payment a simpler and better way to match primary care payments to patients’ needs?
- Won’t paying for acute care visits encourage primary care practices to deliver unnecessary office visits?
- Is Patient-Centered Primary Care Payment consistent with the recommendations on primary care made by the National Academy of Sciences, Engineering, and Medicine?
- How does Patient-Centered Primary Care Payment differ from the hybrid payments in other primary care payment programs, such as the CMMI Primary Care First demonstration?
- Would Patient-Centered Primary Care Payment help reduce the shortage of primary care physicians?
- If primary care physicians have fewer patients under Patient-Centered Primary Care Payment, won’t that make it harder for patients to find a primary care physician?
- Would Patient-Centered Primary Care Payment increase or reduce disparities in access to primary care for disadvantaged individuals and communities?
- How would Patient-Centered Primary Care Payment affect primary care physicians who are employed by large physician groups and health systems and who receive a salary rather than being paid through fees for services?
- How does Patient-Centered Primary Care Payment differ from Direct Primary Care?
- Would Patient-Centered Primary Care Payment support delivery of integrated behavioral healthcare services by primary care practices?
- Would Patient-Centered Primary Care Payment support delivery of telehealth and digital healthcare services by primary care practices?
- How difficult will it be for primary care practices and health insurance plans to implement Patient-Centered Primary Care Payment?
- How would a health plan verify that a patient had enrolled for wellness care or for chronic condition management services?
- What if patients aren’t willing to enroll?
- How would primary care practices be paid for “snowbirds” and other patients who live in different places during different parts of the year?
- How much would insured patients have to pay for services under Patient-Centered Primary Care Payment?
- How does Patient-Centered Primary Care Payment ensure patients are receiving high-quality care?
- How would a patient or payer know that a primary care practice is delivering high-quality care if it is not reporting on quality measures and if its payments are not affected by its performance on those measures?
- Will Patient-Centered Primary Care Payment reduce health care spending?
- Why wouldn’t health insurance plans want to implement Patient-Centered Primary Care Payment?
- Is there a target for the percentage of a health plan’s spending that should be devoted to Patient-Centered Primary Care Payment?
How would a primary care practice be paid under Patient-Centered Primary Care Payment?
In Patient-Centered Primary Care Payment, most of the revenue in a primary care practice would come from three new payments:
- Monthly Payments for Wellness Care. The primary care practice would receive a monthly payment for each patient. This payment would enable the primary care team to deliver wellness care management services, including ensuring that patients are up-to-date on all evidence-based preventive care.
- Monthly Payments for Chronic Condition Management. The primary care practice would receive an additional monthly payment for each patient who has one or more chronic conditions. This payment would enable a primary care team to deliver proactive, evidence-based chronic disease treatment and care management services to the patient. The payment would be higher for patients with a complex condition.
- An Acute Care Visit Fee. In addition to the monthly payment(s), the primary care practice would receive an Acute Care Visit Fee if a patient experiences a new acute health problem and the practice provides evidence-based diagnosis and treatment services to address it. The services could be delivered in whatever way is most appropriate in the circumstances, including by telephone, telehealth, or an in-person visit with the physician or other clinician.
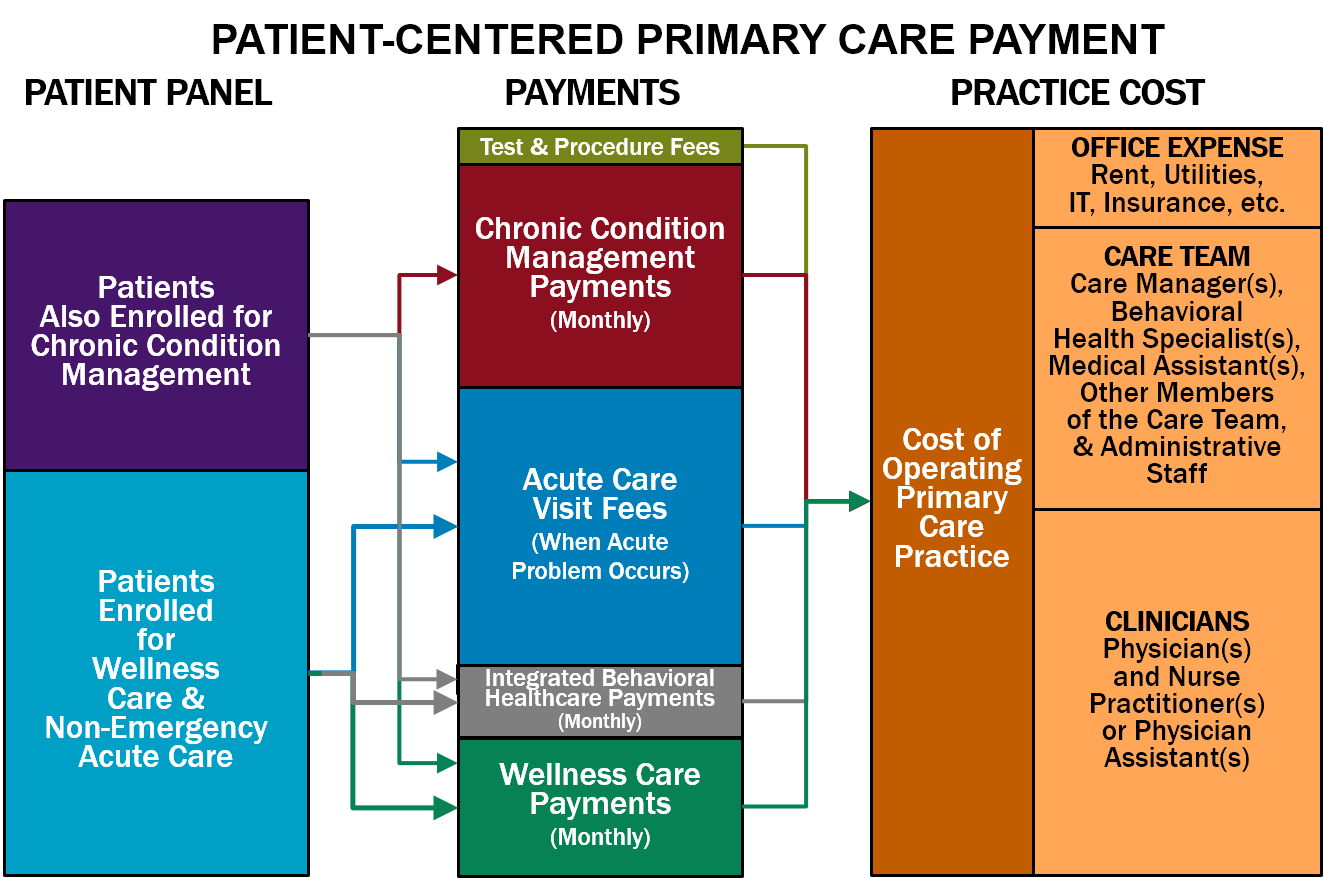
These payments would replace over two dozen separate fees that are currently paid for evaluation and management services to established patients, wellness visits, and chronic condition management. Practices that deliver additional services would receive two additional types of payments:
- Monthly Payments for Integrated Behavioral Healthcare Services Primary care practices that deliver integrated behavioral health services to their patients need to employ or contract with staff who have training in helping patients with behavioral health needs. In order to support this, the practice should receive an additional monthly payment for each patient who has enrolled to receive wellness care from the practice.
- Fees for Individual Procedures and Tests. Many primary care practices also perform procedures such as an immunization, injection, or excision and/or perform basic laboratory tests. It is beneficial for patients to be able to receive these procedures and tests from the practice, rather than needing to make a separate trip to another physician or facility. Since only a subset of patients will need these procedures and tests, and since the cost of performing each of them will differ, the primary care practice should receive an additional fee when it performs a procedure or test that is adequate to cover the cost.
Wouldn’t it be simpler to pay primary care practices using a single per-member-per-month payment rather than three separate payments?
It might be simpler to use a single payment, but it wouldn’t be better, because it would not be a patient-centered payment system. Some patients have more health problems than others, and the primary care practice will need to spend more time with those patients. Paying a single amount for every patient, regardless of the patient’s needs, would penalize a practice financially if it cares for higher-need patients.
Most primary care payment models use multiple payments rather than one single monthly payment. In the Comprehensive Primary Care Plus demonstration project created by the Center for Medicare and Medicaid Innovation (CMMI), primary care practices receive three new payments (a Care Management Fee, a Comprehensive Primary Care Payment, and a Performance-Based Incentive Payment) in addition to all existing fees for office visits, and in the CMMI Primary Care First demonstration project, primary care practices receive two new payments (a Professional Population-Based Payment and a Flat Visit Fee) plus a large performance-based adjustment.
Isn’t a risk-adjusted capitation or population-based payment a simpler and better way to match primary care payments to patients’ needs?
Standard risk adjustment systems, such as the Hierarchical Condition Category (HCC) risk adjustment system used in Medicare payment programs, only adjust payments based on a patient’s age, gender, and the chronic diseases the patient had been diagnosed with prior to the beginning of the year. There is no adjustment in payment for newly diagnosed chronic conditions, for acute health problems the patient experiences during the year, or for non-medical challenges facing a patient such as poverty, homelessness, illiteracy, lack of access to transportation or fresh food, etc. Under these systems, a primary care practice will be penalized financially if it accepts new patients with previously undiagnosed chronic diseases, social challenges, or frequent acute problems.
In contrast, Patient-Centered Primary Care Payment explicitly provides higher payments to a primary care practice for patients who have both new and pre-existing chronic conditions, patients who have multiple acute problems, and patients who have non-medical characteristics that make their care more complicated.
Won’t paying for acute care visits encourage primary care practices to deliver unnecessary office visits?
Under Patient-Centered Primary Care Payment, a primary care practice would only receive an additional payment for an office visit if the patient has a new acute problem that requires attention. If a patient needs to make an office visit for reasons related to preventive care or care for a chronic condition, there would be no additional payment, because the practice would be receiving a monthly payment to provide wellness care or chronic condition management, including any office visits needed for those types of care. If the patient does not have an acute problem, there would be no basis for scheduling an acute care visit that would be eligible for additional payment. Since most patients would have to pay a co-payment for the visit if they have insurance, there would be no reason for the patient to schedule a visit if they did not feel they needed it.
Is Patient-Centered Primary Care Payment consistent with the recommendations on primary care made by the National Academy of Sciences, Engineering, and Medicine?
The May 2021 report from the National Academy of Sciences, Engineering, and Medicine (NASEM), Implementing High-Quality Primary Care: Rebuilding the Foundation of Health Care, recommends that payers use a “hybrid reimbursement model (part FFS, part capitated)” that pays “prospectively for interprofessional, integrated, team-based care” and is “risk adjusted for medical and social complexity.” The report does not define exactly how this hybrid payment model should be structured.
Patient-Centered Primary Care Payment is consistent with this recommendation. It is a “hybrid” payment model, since it uses a combination of (1) per patient per month (“capitation”) payments for Wellness Care and Chronic Disease Management and (2) fees for Acute Care Visits. The Wellness Care and Chronic Condition Management Payments are prospective payments and allow services to be delivered through team-based care approaches. Payments are risk-adjusted for both medical and social complexity, since the practice receives higher total payments for patients who have acute medical problems, chronic diseases, and/or social characteristics that make their care more complex.
How does Patient-Centered Primary Care Payment differ from the hybrid payments in other primary care payment programs, such as the CMMI Primary Care First demonstration?
There are several ways in which Patient-Centered Primary Care Payment differs from the Primary Care First demonstration project designed by the Center for Medicare and Medicaid Innovation (CMMI) and other current hybrid payment models:
- Fees for New Acute Problems Rather Than All Office Visits. Current hybrid payment models for primary care, including Primary Care First, continue to pay a fee for every office visit, including visits for exacerbations of a chronic disease, visits to address preventive care needs, and repeat visits for acute problems that were not adequately addressed the first time. As a result, if the primary care practice helps patients avoid chronic disease exacerbations, if it can ensure patients receive appropriate preventive care through telephone or email contacts with nurses or medical assistants rather than asking a patient to come to the primary care office, or if it can address an acute problem effectively in a single visit, the primary care practice is penalized financially by a reduction in office visit revenues. In contrast, under Patient-Centered Primary Care Payment, the primary care practice only receives a separate fee for an office visit if a patient has a new acute problem, so there is no such penalty.
- Monthly Payments Based on Voluntary Enrollment Rather Than Attribution Based on Recent Office Visits. In addition to fees for office visits, Primary Care First and other current hybrid payment models provide a flexible monthly payment for each “attributed” patient. However, a patient is only attributed to the practice if, during a “lookback period,” the patient made more office visits to the practice than to other primary care providers. As a result, if a primary care practice takes on a new patient, the patient will not be attributed to the practice until some point in the future when the patient has made more office visits to the new practice than to the primary care practice(s) where the patient previously received services. Moreover, if the practice can address the patient’s health needs with few or no office visits, the patient might not be attributed to the practice, in which case there would be no monthly payment for that patient. In contrast, under Patient-Centered Primary Care Payment, the practice could immediately enroll a new patient and receive monthly payments to support their care regardless of how many office visits they make.
- A Higher Monthly Payment for a Complex Patient. The monthly payments in the hybrid payment models used by many insurance plans are not adjusted based on patient needs at all, and if they are, the adjustments are based only on the chronic conditions a patient was diagnosed with in prior years, not on non-medical factors such as poverty, homelessness, illiteracy, or lack of access to transportation that can make their care far more complex. In the CMMI Primary Care First payment model, there is no difference in the monthly payment for an individual patient based on their specific characteristics; instead, the monthly payments to a primary care practice for all patients are higher if the average risk score for all patients in the practice is significantly higher than the average for most primary care practices. In contrast, in Patient-Centered Primary Care Payment, the practice receives a higher payment for each patient who has a chronic condition that requires proactive management, and it receives a much higher payment for a patient who has a complex condition.
Would Patient-Centered Primary Care Payment help reduce the shortage of primary care physicians?
Patient-Centered Primary Care Payment would make practicing primary care more attractive for physicians in several ways:
- Smaller patient panels and more time with patients. The payment amounts would be designed to provide adequate revenues to support a primary care practice with fewer patients than today. This allows physicians to spend more time with patients and ensure they are diagnosing and treating the patients appropriately.
- Ability to deliver care in different ways. The payments would not be restricted to in-person office visits with physicians. Physicians would be able to provide care through telehealth and other digital methods, and to have a team of nurses, medical assistants, and other staff provide services to patients when appropriate.
- Less administrative burden. The physician would not be forced to spend time tracking irrelevant quality measures or requesting prior authorizations in order to order or deliver tests and services that patients need.
- Adequate compensation and reasonable work hours. The payment amounts would be large enough to enable the physician to earn an adequate salary and for the practice to pay competitive salaries and benefits for an appropriately-sized primary care team. The combination of smaller patient panel size and reduced administrative burden would enable the physician to provide the services all of the patients need within a 40-50-hour work week.
If primary care physicians have fewer patients under Patient-Centered Primary Care Payment, won’t that make it harder for patients to find a primary care physician?
There are already shortages of primary care physicians in many communities because the serious problems with current payment systems are discouraging doctors from becoming primary care physicians and causing existing primary care physicians to retire early or simply stop practicing. Moreover, finding a primary care physician today does not assure that the patient will receive good primary care, because primary care physicians do not have adequate time or appropriate staff to provide high-quality care. This is particularly true for patients with complex conditions, since they will require far more time and attention than a primary care practice can afford to provide under current payment systems.
If primary care physicians are paid in a way that enables them to provide high-quality care to patients within a reasonable workday, with fewer administrative burdens, and at a good salary, fewer existing physicians will stop practicing, and more physicians will enter primary care, thereby improving access for patients. Moreover, by enabling physicians to employ and utilize a primary care team to deliver services, they will be able to provide high-quality care to a larger patient panel than they would if they were only paid for the services they themselves deliver.
Would Patient-Centered Primary Care Payment increase or reduce disparities in access to primary care for disadvantaged individuals and communities?
Current payment systems can financially harm primary care practices that care for disadvantaged patients, since the fee amounts are not adequate to support the extra time these patients may need, and quality measurement systems penalize the practice if the patients cannot afford medications or face greater challenges in managing their health problems. This can make it more difficult for disadvantaged patients to find a primary care practice willing to accept them or a practice that is able to provide them with adequate care.
In contrast, under Patient-Centered Primary Care Payment, a primary care practice would receive a higher monthly payment for a patient who has characteristics that make standard approaches to treatment and management of their health problems more difficult, such as inability to afford medications, lack of access to transportation, etc. This will enable the practice staff to devote additional time and attention to the patient. In addition, all of the payments give the practice the flexibility to deliver care in whatever way works best for the patient (in-person, by telephone, and using different members of the primary care team).
How would Patient-Centered Primary Care Payment affect primary care physicians who are employed by large physician groups and health systems and who receive a salary rather than being paid through fees for services?
If a primary care physician receives a salary from an entity such as a medical group or health system, the majority of the revenue to support the salary will still come from the fees paid for the physician’s services. Most such “salaries” are not fixed amounts, but are tied directly or indirectly to the number and types of billable services the physician delivers during the year. As a result, under current payment systems, the employed physician may have the same pressure to see large numbers of patients for short amounts of time as an independent physician would.
If the salary is higher than what the physician could earn practicing independently, it is often because the medical group or health system is subsidizing the salary with profits made on ancillary services the physician orders (such as lab tests and imaging studies) or referrals made to specialists. If so, the primary care physician may be pressured to order unnecessary tests or make unnecessary referrals in order to generate the revenues used for the subsidy.
Under Patient-Centered Primary Care Payment, the group or health system would receive sufficient revenue to pay an adequate salary to the physician without expecting the physician to manage an unreasonably large number of patients, to order unnecessary tests, or to make unnecessary referrals. Moreover, the physician would be able to earn an adequate income without the need to work for a large medical group or health system if they wished to do so.
How does Patient-Centered Primary Care Payment differ from Direct Primary Care?
In the Direct Primary Care model, the physician charges each patient a single monthly fee rather than being paid fees for office visits. Over the course of a year, these monthly fees produce significantly more revenue than the primary care practice would have received from standard fees, which enables the physician to have a much smaller patient panel than in other primary care practices.
However, Direct Primary Care practices don’t accept payments from health insurance plans, which means that the practice can only enroll patients who can afford to pay the full amount of the monthly fees without using insurance. Since the fees typically charged in Direct Primary Care average $65-85 per month for adults, this requires the patient to pay $800 - $1,000 per year out of pocket. As a result, Direct Primary Care practices often struggle to attract and retain an adequate number of patients, even though fewer patients are needed than in a practice supported by standard fee-for-service payments. Moreover, for a healthy patient, the monthly fees add up to much more than what the patient would pay for a few office visits, so the Direct Primary Care practice may have more difficulty attracting healthy patients than patients who need frequent primary care services.
Patient-Centered Primary Care Payment would represent an alternative way for Direct Primary Care Practices to charge for their services that would better align the patient’s financial obligation with the cost of the services the practice is delivering, while still enabling the primary care physician to manage a more reasonably-sized group of patients. Moreover, if Patient-Centered Primary Care Payment is implemented by a health plan without the administrative burdens typically imposed by health plans, the primary care practice should also be willing to accept insurance, thereby expanding access to Direct Primary Care for a broader range of patients.
Would Patient-Centered Primary Care Payment support delivery of integrated behavioral healthcare services by primary care practices?
Under Patient-Centered Primary Care Payment, a primary care practice that delivers integrated behavioral healthcare services would receive a monthly Integrated Behavioral Healthcare Payment for each of the patients who has enrolled for wellness care from the practice. This would be paid in addition to the monthly Wellness Care Payment. The amount of the payment would be sufficient to enable the primary care team to employ a sufficient number of individuals with behavioral health expertise who can provide in-person and/or virtual counseling and care management to patients with a suspected or diagnosed behavioral health problem such as depression, anxiety, or substance use disorder.
Would Patient-Centered Primary Care Payment support delivery of telehealth and digital healthcare services by primary care practices?
Under Patient-Centered Primary Care Payment, the primary care practice would have the flexibility to deliver services to patients in whatever way is most feasible and appropriate for that patient – in person (either at the office or at the patient’s home), by video to the patient’s home, by telephone, by email, or by other electronic methods. Rather than fragmenting the patient’s care as many telehealth-only providers can do, Patient-Centered Primary Care Payment would enable the primary care practice to deliver digital healthcare services in an integrated way, seeing the patient through an appropriate combination of in-person and remote services.
How difficult will it be for primary care practices and health insurance plans to implement Patient-Centered Primary Care Payment?
Patient-Centered Primary Care Payment can be easily implemented using the existing billing systems used by every primary care practice and the claims payment systems used by every health plan. The primary care practice will use CPT codes to bill the health plan for the monthly Wellness Care, Integrated Behavioral Healthcare, and Chronic Condition Management Payments and for Acute Care Visit Fees, just as it bills for services today, and the health plan will pay the primary care practice the appropriate amounts for each of those CPT codes just it as it pays for current services today. In contrast to other hybrid and population-based payment systems, there is no need for attribution systems, risk adjustment, or performance-based adjustments to payments in Patient-Centered Primary Care Payment.
How would a health plan verify that a patient had enrolled for wellness care or for chronic condition management services?
If a patient enrolls with a primary care practice for wellness care or chronic condition management services, the primary care practice would bill the health plan each month for a Wellness Care and/or Chronic Condition Management Payment. When the practice submits a claim to the health plan with a CPT code for one of those payments, the practice would be certifying to the health plan that the patient had enrolled for that type of care and that the patient had received the appropriate services. The primary care practice would maintain documentation that the patient had agreed to enroll.
This is the same approach the Centers for Medicare and Medicaid Services (CMS) is currently using to pay physician practices for chronic condition management (CCM) services to Medicare beneficiaries. According to the CMS guidance document:
A practitioner must obtain patient consent before furnishing or billing CCM. Consent may be verbal or written but must be documented in the medical record, and includes informing them about:
- The availability of CCM services and applicable cost sharing
- That only one practitioner can furnish and be paid for CCM services during a calendar month
- The right to stop CCM services at any time (effective at the end of the calendar month)
Informed patient consent need only be obtained once prior to furnishing CCM, or if the patient chooses to change the practitioner who will furnish and bill CCM.
What if patients aren’t willing to enroll?
Enrollment would enable the patient to receive additional services from the primary care practice and to receive services in more flexible ways than if they do not enroll. Enrolling for wellness care or chronic condition management services would not “lock in” the patient to that practice; the patient could unenroll at any time. Moreover, enrolling would not mean that the practice would serve as a “gatekeeper” for services delivered by other healthcare providers. The patient could still make a visit to another primary care practice or specialist if they wished to, and they would not be required to receive approval from the primary care practice before receiving services from specialists.
It would be up to the primary care practice whether it wanted to continue providing services to a patient who is not willing to enroll for wellness care, since the practice would only be able to receive standard fee-for-service payments for that patient, and it would be unable to provide the same services or the same quality of care to the patient as it was providing to its enrolled patients.
If a patient with a chronic disease wanted to receive care for that disease from a specialist instead of the primary care practice, the patient could still choose to enroll with the primary care practice for wellness care services and care for acute problems, but not to enroll for chronic condition management. If the primary care practice was agreeable to this, it could limit its services to wellness care and acute care, and, with the patient’s permission, it could stay in contact with the specialist practice to share any information necessary to coordinate their respective services appropriately.
How would primary care practices be paid for “snowbirds” and other patients who live in different places during different parts of the year?
Because Patient-Centered Primary Care Payment would allow services to be delivered virtually when appropriate, some patients could receive wellness care and chronic condition management services from their primary care practice even if they are living in another community for a few months. If one of those patients had an acute problem that could not be addressed through telehealth, the patient could seek care from a primary care practice in the community they are visiting, and that practice would be paid for the acute care at standard fee-for-service rates.
Alternatively, the individual could enroll with a primary care practice located in Community A during the portion of the year they reside there. When they move to Community B, they would unenroll from the first practice and enroll in a primary care practice located in Community B, and then reverse the process when they return to Community A. The patient could authorize the two primary care practices to share information in order to ensure continuity of care.
In contrast, the attribution systems currently used by Medicare and other payers assign patients to practices based on where they made the majority of their office visits during a “lookback” period. This can potentially result in the patient being attributed to the primary care practice in Community A after they have returned to Community B and vice versa, or being attributed to one of the practices for the entire year even though the patient is receiving services from a different practice during a portion of the year.
How much would insured patients have to pay for services under Patient-Centered Primary Care Payment?
If a patient has insurance, there should be no patient cost-sharing for the monthly Wellness Care Payments or Chronic Condition Management Payments, nor should they be subject to any deductible. The goal of these services is to prevent health problems from occurring, so it would be undesirable to create cost barriers that could discourage patients from enrolling to receive these services. A modest copayment would be required for an Acute Care Visit Fee in order to discourage patients from making unnecessary visits to the practice, but the copayment amount should be low enough that patients do not avoid contacting the practice when they have an acute issue that should receive attention.
How does Patient-Centered Primary Care Payment ensure patients are receiving high-quality care?
Under Patient-Centered Primary Care Payment, the primary care practice would not be paid for a month of care or an acute care visit with a patient unless the practice had followed evidence-based clinical guidelines for care of the specific health needs of that individual patient during the month or visit (except in cases where the patient was unwilling or unable to use the recommended services). As a result, every patient could be assured that they would receive appropriate care for their specific, individual needs.
How would a patient or payer know that a primary care practice is delivering high-quality care if it is not reporting on quality measures and if its payments are not affected by its performance on those measures?
The quality measures being used in current primary care payment programs and other “value-based payment” systems do not tell a patient or payer whether a primary care practice is delivering high-quality care.
- No primary care practice can achieve 100% success on the quality measures typically used today because the quality measures are not applicable to all of the patients who are measured, and the primary care practice cannot control all of the factors that affect the measure even for those patients for whom the measure is applicable.
- Even if a practice has a 90% score on a quality measure, an individual patient has no assurance that they will be among the 90% who receive care that meets the quality standard versus the 10% who don’t.
- If a practice has a higher percentage score on a quality measure, it may be because the measure is applicable to a higher percentage of patients or that a higher percentage of patients are willing and able to do what is needed, not because the primary care practice staff are delivering care in a different way. Moreover, the fact that a high percentage of patients in a practice have been receiving care consistent with the quality measure does not mean that new patients will.
- Current value-based payment systems have no quality measures at all for the care that many types of patients receive, particularly for acute conditions. The fact that a primary care practice delivers some services in a high-quality way does not guarantee that they will deliver all services that way.
Under Patient-Centered Primary Care Payment, the primary care physician would utilize evidence-based clinical practice guidelines to determine what treatment and management services are most likely to achieve the best outcomes for each individual patient, and the patient would be able to see what services are recommended in the guidelines so they could be sure they were receiving appropriate care. The physician would have the flexibility to deviate from the guidelines in situations where the recommended treatment cannot be used for a particular patient or the patient is unwilling to use that approach, but the reasons for deviation would have to be documented in the patient’s clinical record.
If a health plan was concerned that a primary care practice was not following evidence-based guidelines appropriately, it could request documentation from that practice and recoup any payments that were made inappropriately. This is the same process used today if there is concern that a practice is billing for services inappropriately. In contrast to current quality measurement and prior authorization systems that create enormous burdens for the vast majority of primary care practices that are delivering care appropriately, this approach would focus quality assurance time and costs on practices that are not delivering appropriate and high-quality care.
Will Patient-Centered Primary Care Payment reduce health care spending?
The goal of primary care is to improve patients’ health, not to reduce healthcare spending. Since many patients currently receive poor quality primary care, unnecessary specialty services, and unnecessarily expensive treatments, improving the quality of primary care will likely result in some reduction in spending on other kinds of services for many groups of patients. However, for healthy individuals, better access to higher-quality primary care could easily cause an increase in total healthcare spending, because a higher percentage of those individuals would likely receive appropriate screenings for cancer (e.g., colonoscopies and mammograms), and a higher percentage would use appropriate medications needed to manage chronic conditions (e.g., medications to control cholesterol and blood sugar) and receive regular testing to monitor those conditions. Greater use of these services and medications is important for achieving better health outcomes for the patients, but the payments for these services will increase total healthcare spending, at least in the short run. As a result, one cannot assume that the savings from better care will completely offset the increase in spending needed to provide adequate support for primary care.
Current payments for primary care are forcing many primary care practices to close and new physicians are being discouraged from entering the field. If access to primary care is significantly reduced, it is likely that spending on other services will increase, both in the short run and the long run. As a result, failing to implement Patient-Centered Primary Care Payment could cause healthcare spending to increase even more.
Why wouldn’t health insurance plans want to implement Patient-Centered Primary Care Payment?
Unfortunately, most health insurance plans have been unwilling to implement significantly better payments for primary care practices. The reasons are financial. Spending more on primary care will reduce a health insurance plan’s profits. Even if the plan is simply paying claims for a self-insured employer, the plan will not want to incur any additional administrative costs to implement a new payment system.
In addition, health plans benefit from being free riders. Primary care practices are not going to deliver care differently to patients based on the type of insurance they have, so if other payers pay differently and primary care practices change the way they deliver care in response to those payers, the patients who are members of the non-participating plan will also get better care but the plan won’t incur the extra costs of paying adequately for services.
The strongest and perhaps only economic incentive for a health insurance plan to pay differently for primary care will be if it believes that doing so would significantly increase its membership or that failure to do so would cause it to lose a large number of customers. Consequently, it will be essential for employers and individuals to choose health insurance plans that pay primary care practices using Patient-Centered Primary Care Payment.
Is there a target for the percentage of a health plan’s spending that should be devoted to Patient-Centered Primary Care Payment?
It is both inappropriate and problematic to set targets for the percentage of total healthcare spending that primary care practices should receive. No matter what target amount is used, it may be too low or too high depending on the characteristics of the patient population and the community where they are receiving care. Moreover, if a payer implements other initiatives to reduce utilization rates or payment amounts for specialty services that cause total healthcare spending to decrease, this does not mean that payments for primary care should be reduced in order to maintain the same percentage spending.
Spending on primary care will only be adequate if the amounts paid for primary care services are sufficient to allow primary care practices to spend adequate time and hire the appropriate staff to deliver those services. That is the appropriate criterion for determining whether primary care payments are adequate, not the percentage of total spending going to primary care.